NEWS AND UPDATES
This week, the Federal Trade Commission issued a binding consent order against Express Scripts and its parent company, Cigna.
It wasn’t guidance. It wasn’t symbolic.
The massive budget reconciliation bill known as the One Big Beautiful Bill Act (OBBBA) was signed into law by President Trump on July 4, 2025. As with many such budget bills, there were various employee benefits provisions tucked into its depths, including changes for health savings accounts (HSAs), dependent care assistance programs (DCAPs), student loan payments under educational assistance programs, and qualified transportation plans. The benefit-related changes are summarized below.
A recent legal memo outlines a clear, compliant path forward, rooted in IRS Publication 969, to keep telehealth free for employees in 2025 and beyond. Here’s what you need to know as of March 5, 2025, and how to act on it.
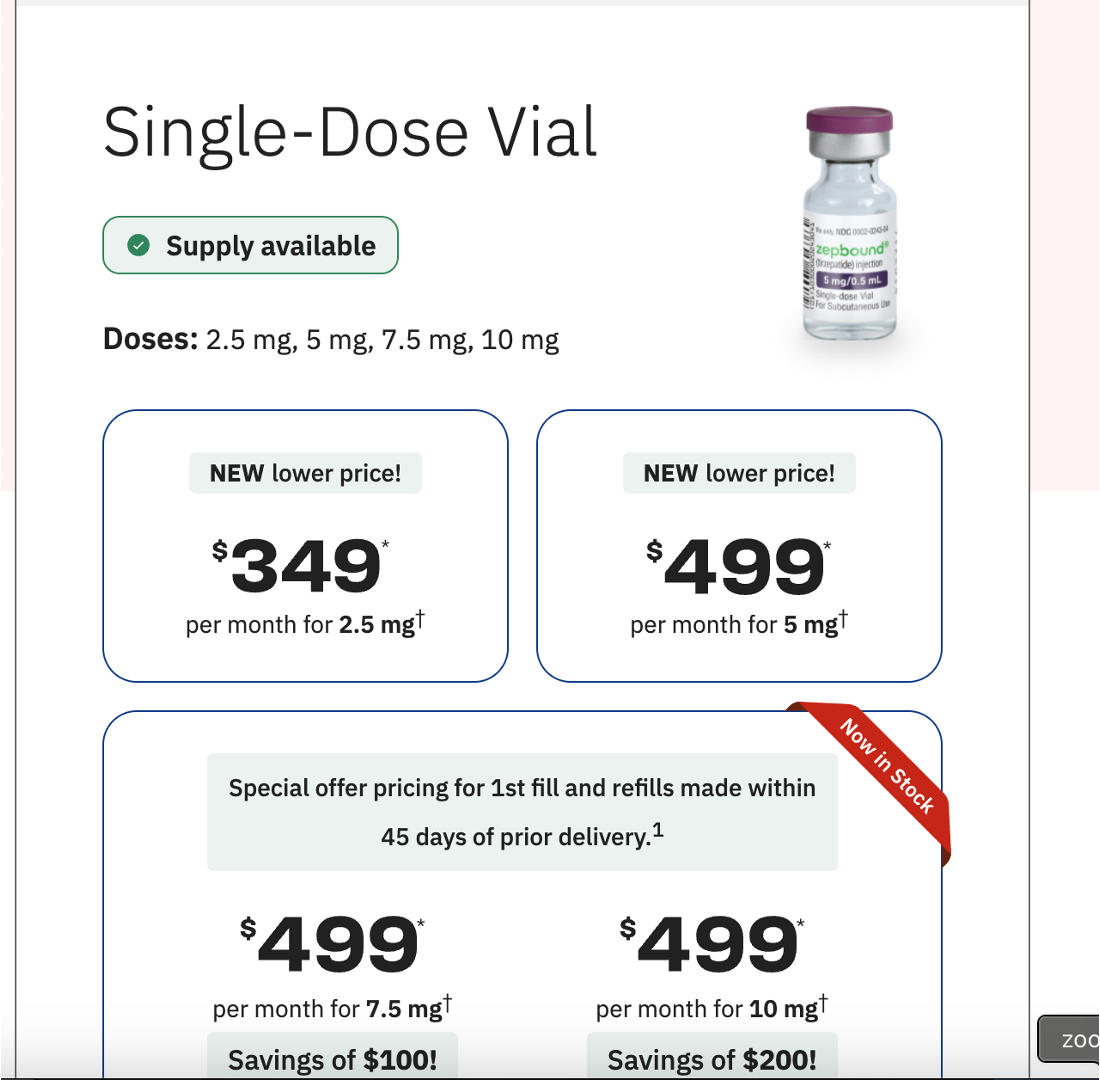
On the heels of the FDA’s announcement ending the drug shortage of popular GLP1s, Wegovy and Ozempic, we have Eli Lilly announcing new and reduced cash-pay pricing for Zepbound.
On February 21, 2025, the U.S. Food and Drug Administration (FDA) announced that the shortage of semaglutide injection products, including Ozempic and Wegovy, has been resolved.
The thing about being a fiduciary is that all responsibility and liability rests on the plan sponsor. You can hire some pretty awful vendors to manage components of your health plan but mismanagement, excess fees, self-dealing, and profiteering are the plan sponsors peril.
It’s like the flood gates have opened and all at once what a few of us have been screaming about for years is all of a sudden coming into sharp focus. The class action lawsuits are here and this is a Big One.
Alarming industry news today of a large regional TPA shuttering operations abruptly endangering access to critical healthcare services and placing plan sponsors in limbo.
“The job of the PBM is to reduce drug costs. Instead they frequency do the opposite.”
Knowing how your PBM makes money is likely the most important component to optimizing your health plan’s Rx spend.
Simpara is announcing that four of their esteemed clients will be honored by Health Rosetta Institute for providing employees one of “America’s Top 50 Health Plans.”
Our Humira-Watch continues as a flood of biosimilars hit the market. Some of these drug options cost 85% less than Humira.
While Americans are enjoying the long holiday break the first interchangeable Rx for Humira quietly launched July 1, 2023 - this means the pharmacy can dispense Cyltezo, the cheaper biosimilar, without a new script.
In a quiet announcement last week, CMS issued a new set of FAQs related to Gag Clause Prohibitions – a provision included in the Consolidated Appropriations Act of 2021.
Amjevita, the first biosimilar competitor to Humira hit the U.S. market at the end of January. Showcasing the dysfunction of our healthcare delivery system, the copycat drug came to market with two drastically different list prices. One, a mere 5% discount relative to Humira and another with a 55% discount. Why two prices and who would pay for the more expensive option?
The Department of Labor gave employers an early Christmas gift last week by issuing a new set of FAQs related to the Consolidated Appropriations Act (CAA) and specifically the new health plan reporting requirements.
We’re hearing rumors from industry insiders that the OMB is set to issue regulations which aim to fix the so-called ACA “Family Glitch” as soon as this coming week. The new rules could take effect as early as November 1, 2022 - just in time for Open Enrollment 2023.
For middle-aged men, 1 in 4 suffers from Obstructive Sleep Apnea (17% for women). The average cost for an in-lab sleep study, used to determine and diagnose sleep apnea is $5,384. A high price tag for a diagnosis which may turn up negative.
In 2003, a little drug named Humira hit the market under the name DE27. Analysts believed at the time that Humira, which was approved to treat Rheumatoid Arthritis, would eventually generate between $500M and $1B in sales annually. In 2021, Humira’s global sales totaled $20.7B. Lifetime earnings have eclipsed $200B.
Last week, the Supreme Court made their decision in Marietta Memorial Hospital Employee Health Benefit Plan v. DaVita Inc., resulting in a 7-2 vote against the major dialysis provider.
Starting in July 2022, the nation’s three largest credit bureaus – Equifax, Experian and TransUnion – will be removing nearly 70% of medical debt in collections accounts from credit reports.
On April 12, 2022, True Captive Insurance will be hosting The Future of Business & Benefits – St. Louis event at Busch Stadium, where local business leaders will discuss employee healthcare trends, self-funding health plans and how to gain control of healthcare spend.
Companies enhancing patient access to care and lowering patient costs all while slashing their own costs? That’s what earns Health Plan Hero status.
The latest in the string of ongoing lawsuits involving opioids has the epidemic making headlines once again. And industry experts like Health Rosetta co-founder Dave Chase share strategies for addressing it once and for all.






























Hidden no more. The Employers’ Forum of Indiana (EFI) is giving people a look behind the curtain at the reality of hospital costs in the United States.
What began as the first hospital price transparency study in the U.S., commissioned by EFI and conducted by RAND Corporation back in 2017, eventually became the foundation for the Employer Hospital Price Transparency Project.